By: Hera Daria
Lisa* (age 17) said:
I could look in the mirror and not feel like it was me […] I knew it was me, but I didn’t feel like it was me.
Verity* (age 14) explained:
I’m zoned out and don’t notice what’s going on around me. […] People could be calling my name or waving in my face, and like, I don’t notice.
*Names have been changed to protect privacy.

The Definition of Trauma
Trauma is the lasting emotional response that often results from living through a distressing event. Experiencing a traumatic event can harm a person’s sense of safety, sense of self, and ability to regulate emotions and navigate relationships. Long after the traumatic event occurs, people with trauma can often feel shame, helplessness, powerlessness and intense fear.
A traumatic event can be:
- a recent, single traumatic event (e.g., car crash, violent assault)
- a single traumatic event that occurred in the past (e.g., a sexual assault, the death of an immediate family member, an accident, living through a natural disaster or a war)
- a long-term, chronic pattern (e.g., ongoing childhood neglect, bullying, sexual or physical abuse).
In a nationally representative sample of U.S. adolescents ages 13 to 17 years old, 62% had been exposed to at least one lifetime traumatic event and 19% had been exposed to three or more traumatic events (McLaughlin et al., 2013).
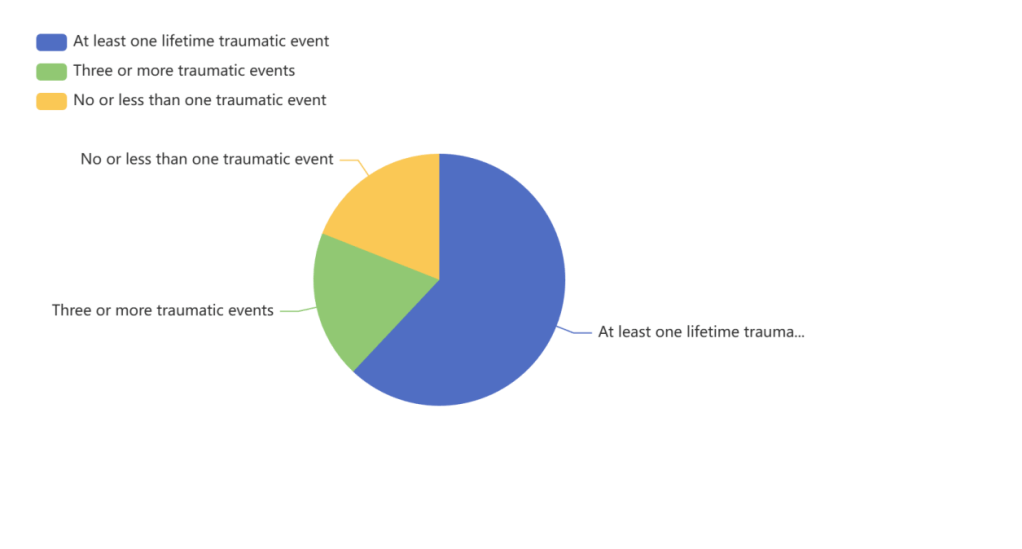
Dissociation as a Response to Trauma
The impact of trauma on an individual is complex, and stress reactions vary considerably. It’s true to say that two people experiencing a similar traumatic event may react in completely different ways.
There are, however, some common responses to trauma. Dissociation is one such response, and this is especially so in cases of extreme physical, emotional and/or sexual abuse or severe neglect. The important thing to understand about dissociation is that it’s a defense mechanism – it is a way the mind copes with the stress of a traumatic event.
Dissociation is a disconnection between a person’s thoughts, feelings, and memories and their sense of self. There is a break in how the mind handles information in response to extreme stress. It involves detaching from reality.
Why dissociation happens has everything to do with protection. It is a built-in coping mechanism that activates when your mind or body feels overwhelmed, unsafe, or unable to process what is happening. In the face of trauma, persistent emotional neglect, or intense stress, the nervous system may shut down certain functions to reduce pain. This disconnection can start early, especially if childhood involved abuse, chaos, or inconsistent care. The brain learns to escape reality by detaching, and this pattern can continue into adulthood. Dissociation can also be triggered by later experiences like accidents, assaults, or grief. It often coexists with anxiety, chronic stress, or PTSD, and can even arise in emotionally exhausting environments where constant overwhelm becomes the norm.
Dissociation can also be experienced as part of a mental health condition, such as schizophrenia, bipolar disorder or borderline personality disorder (BPD).
Dissociation becomes pathological when it is no longer adaptive and impairs normal functioning. And, depending on symptoms and clinical assessment, shows the existence of a dissociative disorder. In dissociative disorders, dissociation is no longer a temporary coping response, but a dominant and disruptive pattern. Dissociative disorders include dissociative amnesia, Depersonalization/Derealization Disorder and Dissociative Identity Disorder (DID).
Dissociative Symptoms in Teens
The teenage years are commonly associated with a lack of focus and mood swings, which makes detecting signs of dissociation that much more difficult. However, certain patterns can be identified, particularly in times of stress, to determine when it is a good time to seek professional assistance.
Common dissociative symptoms in adolescents include:
- Feeling separation from yourself or your emotions – as if you are outside of your life looking in
- Feeling numb
- Feeling disconnected from your physical body
- Believing that you or others around you are not real
- Detachment from your identity
- Inability to cope with the stress of daily life
- Unexplained memory loss or amnesia (especially after emotional conversations or stressful events)
For some teens, these symptoms can come and go quickly, but for others, they can profoundly affect their friendships, grades, confidence, and even their safety. If there is any threat of harm to the person experiencing dissociation or anyone else, we recommend seeking assistance immediately.
Early detection of dissociation in adolescence may be critical, as dissociative disorders often begin with milder symptoms (Lyssenko et al., 2018), and early intervention may lead to faster symptom reduction (Myrick et al., 2012) and reduce the risk of symptom progression (Putnam, 1997; Silberg, 2022).
Complications of Dissociation
Dissociation can create a range of complications that affect your ability to function and feel grounded in daily life. You might find it difficult to concentrate, remember things, or feel emotionally connected to yourself or others. Relationships can become strained, and tasks that once felt simple may suddenly feel overwhelming or disconnected from meaning.
Some common complications of dissociation include:
- Memory gaps or blackouts
- Difficulty concentrating or staying focused
- Emotional numbness or detachment
- Feeling disconnected from your body or surroundings
- Trouble maintaining relationships
- Increased anxiety or depression
- Risk of self-harm or unsafe behavior during episodes
If dissociation is left unaddressed, it can lead to long-term emotional distress and impact your sense of identity. Healing often begins by identifying the cause and working through it in a safe, supportive environment.
How Can We Face Dissociation?
Understanding why dissociation happens is the first step toward healing. It’s not a flaw or weakness; it’s your mind’s way of trying to protect you from something overwhelming. But when dissociation becomes frequent or disruptive, it’s time to seek support. With the right therapeutic approach, you can feel safe in your body again, stay present, and rebuild emotional stability.
Dissociation Treatment:
Early intervention for dissociation in teens is vital. Not only to avoid the development of a disorder, but also to prevent behaviors from becoming dangerous to the teen or to their loved ones. While it can be helpful to talk with a trusted friend, someone at your local faith center, or in a community education group, professional therapy can offer additional emotional support for teens.
Talk Therapy for Dissociative Episodes in Teens:
Talk therapy, also known as psychotherapy, is the most-used treatment method for dissociation in teens. It involves talking about your difficult thoughts, feelings, and behaviors with a licensed mental health professional. Throughout your therapy sessions, your therapist will help you to make sense of your experiences and learn ways to cope. Psychotherapy can take many different forms, and the right approach for you will depend on your preferences and situation. Some of the most common approaches for teens with dissociation include:
- Dialectical Behavior Therapy (DBT) to improve emotional regulation and grounding
- Eye Movement Desensitization and Reprocessing (EMDR) for trauma-related dissociation
- Mindfulness-Based Cognitive Therapy
- Cognitive Behavioral Therapy (CBT) to address thought patterns and triggers
- Somatic therapies to reconnect the mind and body
Medication may be used to treat co-occurring conditions. Healing takes time, but with the right support, you can reduce dissociative episodes and feel more present and in control.
Grounding Techniques for Teen Dissociation:
One of the most effective ways to help a teen with dissociation is to teach them techniques that will ground them in their body. For a teen, it’s not only a way to keep from spiraling, but it is also a way for them to have some autonomy in their experience. This can be everything to adolescents who often feel they have no control over the situations they find themselves in.
Talk about different grounding methods for teens to determine which ones they find most helpful. These can be practiced when the teen is calm and kept as prime coping skills in their self-care toolkit.
Several strategies for coping with dissociation in teens include:
- Breathing deep, slow breaths
- Box breathing – four seconds breathing in, four seconds holding the breath in, four seconds breathing out, and four seconds holding the breath out. Repeat several times.
- Meditation and mindfulness activities
- Pet an animal or touch nature (a tree, grass, dirt, etc.)
- Move your body and stretch
- Use the 5-4-3-2-1 sensory technique – Find five things you can see, four things you can touch, three things you can hear, two things you can smell, and one thing you can taste
- Cold exposure – splash cold water on your face or hold an ice cube
Conclusion:
The brain will always prioritize safety. Emotions need to be processed gradually, at a pace that feels manageable. The environment we heal in must be supportive and patient, because a sense of safety needs time to reach every affected part of us. When it comes to dissociation, grounding and patience are especially important. You are not weak. You are not exaggerating. Trauma places a real burden on the brain, and your responses make sense. Your brain has its own rhythm of processing. Let yourself rest in its hands, giving it the time and space it needs. Being in a safe place where you can work through grief, trauma, and healing is important. Allow yourself to emerge only in spaces that hold safety and care.


Leave a comment